Summary
Objective
Dyslipidemia is frequently observed in patients with obstructive sleep apnea syndrome (OSAS). The effects of OSAS treatment on lipid levels in these patients have been examined.
Patients and Methods
95 consecutive patients (aged 56.6±9.5 years) with polysomnographically verified OSAS and LDL cholesterol levels of more than 130 mg per deciliter have been included in a prospective trial. Plasma total cholesterol, high-density lipoprotein (HDL) cholesterol, low-density lipoprotein (LDL) cholesterol, triglyceride, apolipoprotein B, and lipoprotein (a) levels were determined in all patients at baseline and after long term therapy.
Results
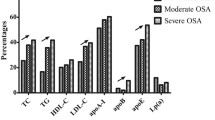
Total cholesterol (249.9±31.4 vs. 240.0±34.1 mg/dL; p=0.01) and LDL cholesterol levels (179.4±29.4 vs. 165.5±32.5 mg/dL; p<0.001) decreased significantly after 6 months in patients effectively treated, while they did not change significantly in those OSAS patients in whom treatment proved to be ineffective. Body mass index, HDL cholesterol, triglyceride, apolipoprotein B, and lipoprotein (a) levels did not change during follow-up. Both the change of total and LDL cholesterol levels were independently associated with treatment efficacy as indicated by the change of the apnea/hypopnea index.
Conclusion
The results suggest that effective treatment of sleep-disordered breathing may have significant effects on the total and LDL cholesterol levels in OSAS patients.
Zusammenfassung
Einführung
Fettstoffwechselstörungen werden häufig bei Patienten mit obstruktivem Schlafapnoe Syndrom (OSAS) beobachtet. Die vorliegende prospektive Studie untersuchte den Einfluß einer schlafmedizinischen Therapie auf den Lipidmetabolismus bei OSAS-Patienten.
Patienten und Methodik
95 konsekutive Patienten (Alter 56.5±9.5 Jahre) mit polysomnographisch gesichertem OSAS und einem LDL-Cholesterinspiegel von >130 mg/dl wurden in die vorliegende Studie aufgenommen. Bei allen Patienten wurden zum Ausgangszeitpunkt und nach einer OSAS-Langzeittherapie Gesamtcholesterin, high-density lipoprotein (HDL) Cholesterin, low-density lipoprotein (LDL) Cholesterin, Triglyzeride, Apolipoprotein B sowei Lipoprotein (a) bestimmt.
Ergebnisse
Das Gesamtcholesterin (249,9±31,4 vs. 240,0±34,1 mg/dl; p=0,01) sowie das LDL-Cholesterin (179,4±29,4 vs. 165,5±32,5 mg/dl; p<0,001) sanken signifikant nach 6 Monaten unter effektiver Therapie, wohingegen sie sich bei den ineffektiv behandelten Patienten nicht signifikant änderten. Der Body Mass Index, das HDL-Cholesterin, die Triglyzeride, das Apolipoprotein B sowie das Lipoprotein (a) blieben im Verlauf unverändert. Sowohl die Änderung des Gesamt-als auch die des LDL-Cholesterins waren unabhängig mit der Therapieeffizienz, gemessen an der Änderung des Apopnoe/Hypopnoe Index (AHI), assoziiert.
Schlussfolgerungen
Diese Ergebnisse deuten darauf hin, dass eine effektive schlafmedizinische Therapie bei OSAS-Patienten einen signifikanten Einfluss auf den Gesamt-und LDL-Cholesterinspiegel ausüben kann.
Similar content being viewed by others
References
American Academy of Sleep Medicine Task Force: Sleep-related breathing disorders in adults: Recommendations for syndrome definition and measurement techniques in clinical research. Sleep 22: 667–689, 1999.
American Thoracie Society—Medical Section of the American Lung Association: Indications and standards for cardiopulmonary sleep studies. Am Rev Respir Dis 139:559–568, 1989.
Bjorntorp P: Obesity. Lancet 350: 423–426, 1997.
Carlson JT, Hedner J, Elam M, et al.: Augmented resting sympathetic activity in awake patients with obstructive sleep apnea. Chest 103: 1763–1768, 1993.
Chin K, Shimizu K, Nakamura T et al.: Changes in intra-abdominal visceral fat and serum leptin levels in patients with obstructive sleep apnea syndrome following nasal continuous positive airway pressure therapy. Circulation 100: 706–712, 1999.
Friedewald WT, Levy RI, Fredrickson DS: Estimation of the concentration of low-density lipoprotein cholesterol in plasma. without use of the preparative ultracentrifuge. Clin Chem 18: 499–502, 1972.
Goldstein JL, Kita T, Brown MS: Defective lipoprotein receptors and atherosclerosis. N Engl J Med 309: 288–296, 1983.
Havel RJ: Biology of cholesterol, lipoproteins and atherosclerosis. Clin Exp Hypertens 11: 887–900, 1989.
He J, Kryger MH, Zorik FJ, et al.: Mortality and apnea index in obstructive sleep apnea. Chest 94: 9–14, 1988.
Howard BV, Schneiderman N, Falkner B, et al.: Insulin, health behaviors, and lipid metabolism. Metabolism 42: Suppl. 1: 25–35, 1993.
Hung J, Whitford EG, Parsons RW, et al. Association of sleep sapnoea with myocardial infarction in men. Lancet 336: 261–264, 1990.
Jenkinson C, Davies RJO, Mullins R, et al.: Comparison of therapeutic and subtherapeutic nasal continuous positive airway pressure for obstructive sleep apnoea: a randomized prospective parallel trial. Lancet 353: 2100–2105, 1999.
Lavie P, Herer P, Peled R, et al.: Mortality in sleep apnea patients: a multivariate analysis of risk factors. Sleep 18: 149–157 1995.
Levine GN, Keaney JF, Vita LA: Cholesterol reduction in cardiovascular disease. N Engl J Med 332: 512–521, 1995.
Mayer J, Becker H, Brandenburg U, et al.: Blood pressure and sleep apnea: results of long-term nasal continuous positive airway pressure therapy. Cardiology 79: 84–92, 1991.
Partinen M, Jamieson A, Guilleminault C: Long-term outcome for obstructive sleep apnea syndrome patients. Chest 94: 1200–1204, 1988.
Rechtschaffen A, Kales A: A manual of standardized terminology, techniques and scoring system for sleep stages of human subjects. Washington, DC, U.S. Government Printing Office, 1968 (NIH publication No. 204).
Sniderman AD, Zhang XI, Cianflone K: Governance of the concentration of plasma LDL: a reevaluation of the LDL receptor paradigm. Atherosclerosis 148: 215–229, 2000.
Somers VK, Dyken ME, Clary MP et al.: Sympathetic neural mechanisms in obstructive sleep apnea. J Clin Invest 96: 1897–1904, 1995.
Suzuki M, Otsuka K, Guilleminault C: Long-term nasal continuous positive airway pressure administration can normalize hypertension in obstructive sleep apnea patients. Sleep 16: 545–549, 1993.
Tang JL, Armitage JM, Lancaster T, et al.: Systematic review of dietary intervention trials to lower blood total cholesterol in free-living subjects. BMJ 316: 1213–1220, 1998.
The Scandinavian Sim vastatin Survival Study Group: Randomized trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandmavian Simvastatin Survival Study (4S). Lancet 344: 1383–1389, 1994.
Tremblay A, Buemann B: Exercise-training, macronutrient balance and body weight control. Int J Obes Relat Metab Disord 19: 79–86, 1995.
Wright J, Johns R, Watt I, et al.: Health effects of obstructive sleep apnoea and the effectiveness of continuous positive airways pressure: a systematic review of the research evidence. BMJ 314: 851–860, 1997.
Young T, Palta M, Dempsey J, et al.: The occurrence of sleepdisordered breathing among middle-aged adults. New Engl J Med 328: 1230–1235, 1993.
Young T, Peppard P, Palta M, et al.: Population-based study of sleep-disordered breathing as a risk factor for hypertension. Arch Intern Med 157: 1746–1752, 1997.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Buechner, N.J., Zidek, W., Eßer, M. et al. Obstructive sleep apnea syndrome. Effects of therapy on dyslipidemia. Somnologie 5, 97–102 (2001). https://doi.org/10.1046/j.1439-054X.2001.01159.x
Issue Date:
DOI: https://doi.org/10.1046/j.1439-054X.2001.01159.x