Abstract
Introduction
Presently, the severity of obstructive sleep apnea (OSA) is estimated based on the apnea-hypopnea index (AHI). Unfortunately, AHI does not provide information on the severity of individual obstruction events. Previously, the severity of individual obstruction events has been suggested to be related to the outcome of the disease. In this study, we incorporate this information into AHI and test whether this novel approach would aid in discriminating patients with the highest risk. We hypothesize that the introduced adjusted AHI parameter provides a valuable supplement to AHI in the diagnosis of the severity of OSA.
Methods
This hypothesis was tested by means of retrospective follow-up (mean ± sd follow-up time 198.2 ± 24.7 months) of 1,068 men originally referred to night polygraphy due to suspected OSA. After exclusion of the 264 patients using CPAP, the remaining 804 patients were divided into normal (AHI < 5) and OSA (AHI ≥ 5) categories based on conventional AHI and adjusted AHI. For a more detailed analysis, the patients were divided into normal, mild, moderate, and severe OSA categories based on conventional AHI and adjusted AHI. Subsequently, the mortality and cardiovascular morbidity in these groups were determined.
Results
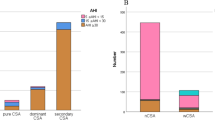
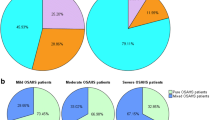
Use of the severity of individual obstruction events for adjustment of AHI led to a significant rearrangement of patients between severity categories. Due to this rearrangement, the number of deceased patients diagnosed to have OSA was increased when adjusted AHI was used as the diagnostic index. Importantly, risk ratios of all-cause mortality and cardiovascular morbidity were higher in moderate and severe OSA groups formed based on the adjusted AHI parameter than in those formed based on conventional AHI.
Conclusions
The adjusted AHI parameter was found to give valuable supplementary information to AHI and to potentially improve the recognition of OSA patients with the highest risk of mortality or cardiovascular morbidity.





Similar content being viewed by others
References
Phillipson EA (1993) Sleep apnea—a major public health problem. N Engl J Med 328(17):1271–1273
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235
Gami AS, Hodge DO, Herges RM, Olson EJ, Nykodym J, Kara T, Somers VK (2007) Obstructive sleep apnea, obesity, and the risk of incident atrial fibrillation. J Am Coll Cardiol 49(5):565–571
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342(19):1378–1384
Shahar E, Whitney CW, Redline S, Lee ET, Newman AB, Javier Nieto F, O’Connor GT, Boland LL, Schwartz JE, Samet JM (2001) Sleep-disordered breathing and cardiovascular disease: cross-sectional results of the Sleep Heart Health Study. Am J Respir Crit Care Med 163(1):19–25
Somers VK, White DP, Amin R, Abraham WT, Costa F, Culebras A, Daniels S, Floras JS, Hunt CE, Olson LJ, Pickering TG, Russell R, Woo M, Young T (2008) Sleep apnea and cardiovascular disease: an American Heart Association/American College of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council on Cardiovascular Nursing. J Am Coll Cardiol 52(8):686–717
Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, Stubbs R, Hla KM (2008) Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep 31(8):1071–1078
Somers VK, Dyken ME, Mark AL, Abboud FM (1993) Sympathetic-nerve activity during sleep in normal subjects. N Engl J Med 328(5):303–307
Somers VK, Mark A, Abboud DC, Abboud FM (1989) Influence of ventilation and hypocapnia on sympathetic nerve responses to hypoxia in normal humans. J Appl Physiol 67(5):2095–2100
Bradley TD, Floras JS (2003) Sleep apnea and heart failure: Part I: obstructive sleep apnea. Circulation 107(12):1671–1678
AASM (1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The Report of an American Academy of Sleep Medicine Task Force. Sleep 22(5):667–689
Iber C, Ancoli-Israel S, Chesson A, Quan SF, for the American Academy of Sleep Medicine (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. AASM, Darien
Kulkas A, Tiihonen P, Julkunen P, Mervaala E, Töyräs J (2013) Novel parameters indicate significant differences in severity of obstructive sleep apnea with patients having similar apnea-hypopnea index. Med Biol Eng Comput 6:697–708
Muraja-Murro A, Eskola K, Kolari T, Tiihonen P, Hukkanen T, Tuomilehto H, Peltonen M, Mervaala E, Töyräs J (2013) Mortality in middle-aged men with obstructive sleep apnea in Finland. Sleep Breath 17(3):1047–1053
Muraja-Murro A, Nurkkala J, Tiihonen P, Hukkanen T, Tuomilehto H, Kokkarinen J, Mervaala E, Töyräs J (2012) Total duration of apnea and hypopnea events and average desaturation show significant variation in patients with a similar apnea-hypopnea index. J Med Eng Technol 36(8):393–398
Otero A, Felix P, Presedo J, Zamarron C (2012) An evaluation of indexes as support tools in the diagnosis of sleep apnea. Ann Biomed Eng 40(8):1825–1834
Muraja-Murro A, Kulkas A, Hiltunen M, Kupari S, Hukkanen T, Tiihonen P, Mervaala E, Töyräs J (2013) The severity of individual obstruction events is related to increased mortality rate in severe obstruction sleep apnea. J Sleep Res 22(6):663–669. doi:10.1111/jsr.12070
Kulkas A, Tiihonen P, Eskola K, Julkunen P, Mervaala E, Töyräs J (2013) Novel parameters for evaluating severity of sleep disordered breathing and for supporting diagnosis of sleep apnea-hypopnea syndrome. J Med Eng Technol 37(2):135–143
Otero A, Felix P, Presedo J, Zamarron C (2010) Evaluation of an alternative definition for the apnea-hypopnea index. Conf Proc IEEE Eng Med Biol Soc 2010:4654–4657
Punjabi NM, Caffo BS, Goodwin JL, Gottlieb DJ, Newman AB, O’Connor GT, Rapoport DM, Redline S, Resnick HE, Robbins JA, Shahar E, Unruh ML, Samet JM (2009) Sleep-disordered breathing and mortality: a prospective cohort study. PLoS Med 6(8):e1000132
Mediano O, Barcelo A, de la Pena M, Gozal D, Agusti A, Barbe F (2007) Daytime sleepiness and polysomnographic variables in sleep apnoea patients. Eur Respir J 30(1):110–113
Yaggi HK, Concato J, Kernan WN, Lichtman JH, Brass LM, Mohsenin V (2005) Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med 353(19):2034–2041
Valham F, Mooe T, Rabben T, Stenlund H, Wiklund U, Franklin KA (2008) Increased risk of stroke in patients with coronary artery disease and sleep apnea: a 10-year follow-up. Circulation 118(9):955–960
Redline S, Yenokyan G, Gottlieb DJ, Shahar E, O’Connor GT, Resnick HE, Diener-West M, Sanders MH, Wolf PA, Geraghty EM, Ali T, Lebowitz M, Punjabi NM (2010) Obstructive sleep apnea-hypopnea and incident stroke: the sleep heart health study. Am J Respir Crit Care Med 182(2):269–277
Peker Y, Carlson J, Hedner J (2006) Increased incidence of coronary artery disease in sleep apnoea: a long-term follow-up. Eur Respir J 28(3):596–602
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Muraja-Murro, A., Kulkas, A., Hiltunen, M. et al. Adjustment of apnea-hypopnea index with severity of obstruction events enhances detection of sleep apnea patients with the highest risk of severe health consequences. Sleep Breath 18, 641–647 (2014). https://doi.org/10.1007/s11325-013-0927-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-013-0927-z