Abstract
Objective
To evaluate the right ventricular function in patients with obstructive sleep apnea syndrome (OSAS) independent from systemic hypertension (HT) and to determine the association between OSAS severity and right ventricular dysfunction.
Methods
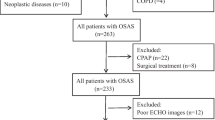
The study population included 77 consecutive subjects; 20 of these patients had OSAS, 20 of them had HT, but did not have OSAS, 16 patients, who constituted the study group, had both disorders, and 21 subjects without any of these two disorders represented the control group. Right ventricular function was assessed by echocardiography: standard two-dimensional, M-Mode, and conventional Doppler as well as tissue Doppler imaging. None of the patients had a previous history of cardiac disease. The diagnosis of OSAS was based on an apnea- hipopnea index of 5 or higher in polysomnography.
Results
Tricuspid inflow velocities and tissue Doppler derived tricuspid annular diastolic velocities were significantly different in the patient groups (OSAS, HT, OSAS + HT) compared to the control group. Tricuspid annular plane systolic excursion (TAPSE) (18.3 ± 3.2, 18.4 ± 2.5, 20.1 ± 2.1, and 20.7 ± 2.5 mm, respectively, P = 0.024) and peak systolic myocardial velocity at tricuspid lateral annulus (S-vel) (12.2 ± 1.5, 10.9 ± 0.9, 11.2 ± 1.1, and 13.1 ± 2.1 cm/s, respectively, P < 0.001) were significantly lower in patient groups compared to those of the study group. Tissue Doppler derived myocardial performance index (MPI) of the right ventricle was significantly impaired in the patient groups compared to the control group (0.34 ± 0.06, 0.44 ± 0.06, 0.45 ± 0.07, and 0.41 ± 0.06, respectively, P < 0.001). With regard to these right ventricular functional parameters, there was no significant difference between OSAS and the other patient groups (HT and OSAS + HT). There were significant correlations both between OSAS severity and the right ventricular functions, and between diastolic and systolic parameters of the right ventricle (r = −0.45, P < 0.05).
Conclusion
Both right ventricular systolic and diastolic functions are impaired in patients having OSAS with or without HT. Right ventricular MPI was found to be the parameter most closely related with OSAS severity and the right ventricular subclinical dysfunction.



Similar content being viewed by others
References
Young T, Peppard PE, Gottlieb DJ (2002) Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med 165:1217–1239
Shahar E, Whitney CW, Redline S, et al (2001) Sleep-disordered breathing and cardiovascular disease cross-sectional results of the sleep heart health study. Am J Respir Crit Care Med 163:19–25
Williams AJ, Houston D, Finberg S, et al (1985) Sleep apnea syndrome and essential hypertension. Am J Cardiol 55:1019–1022
Chaouat A, Weitzenblum E, Krieger J, Oswald M, Kessler R (1996) Pulmonary hemodynamics in the obstructive sleep apnea syndrome: results in 220 consecutive patients. Chest 109:380–386
Kraiczi H, Caidahl K, Samuelsson A, Peker Y, Hedner J (2001) Impairment of vascular endothelial function and left ventricular filling: association with the severity of apnea induced hypoxemia during sleep. Chest 119:1085–1091
Laaban JP, Pascal-Sebaoun S, Bloch E, Orvoen-Frija E, Oppert JM, Huchon G (2002) Left ventricular systolic dysfunction in patients with obstructive sleep apnea syndrome. Chest 122:1133–1138
Alchanatis M, Tourkohoriti G, Kosmas EN, Panoutsopoulos G, Kakouros S, Papadima K, Gaga M, Jordanoglou JB (2002) Evidence for left ventricular dysfunction in patients with obstructive sleep apnoea syndrome. Eur Respir J 20:1239–1245
Nahmias J, Lao R, Karetzky M (1996) Right ventricular dysfunction in obstructive sleep apnoea: reversal with nasal continuous positive airway pressure. Eur Respir J 9(5):945–951
Bradley TD (1992) Right and left ventricular functional impairment and sleep apnea. Clin Chest Med 13:459–479
Berman EJ, DiBenedetto RJ, Causey DE, Mims T, Conneff M, Goodman LS, Rollings RC (1991) Right ventricular hypertrophy detected by echocardiography in patients with newly diagnosed obstructive sleep apnea. Chest 100: 347–350
Severino S, Caso P, Cicala S, Galderisi M, de Simone L, D’Andrea A, D’Errico A, Mininni N (2000) Involvement of right ventricle in left ventricular hypertrophic cardiomyopathy:analysis by pulsed Doppler tissue imaging. Eur J Echocardiogr 1:281–288
Galderisi M, Severino S, Caso P, Cicala S, Petrocelli A, De Simone L, Mininni N, de Divitiis O (2001) Right ventricular myocardial diastolic dysfunction in different kinds of cardiac hypertrophy: analysis by pulsed Doppler tissue imaging. Ital Heart J 2:912–920
Mittal SR, Barar RV, Arora H (2001) Echocardiographic evaluation of left and right ventricular function in mild hypertension. Int J Cardiovasc Imaging 17:263–270
Kales A, Cadieuw RJ, Shaw LC, et al (1984) Sleep apnea in a hypertensive population. Lancet 3:1005–1008
Seward JB, Chan KL (1985) Continuous wave Doppler determination of right ventricular pressure: a simultaneous Doppler catheterization study in 127 patients. J Am Coll Cardiol 6:750–756
Sahn D, DeMaria A, Kisslo J, et al (1978) Recommendations regarding quantification in M-mode echocardiography: results of a survey of echocardiographic measurements. Circulation 58:1072–1083
Naeije R, Torbicki A (1995) More on the noninvasive diagnosis of pulmonary hypertension. Eur Respir J 8:1445–1449
Appleton CP, Jensen JL, Hatle LK, Oh JK (1997) Doppler evaluation of left and right ventricular diastolic function: a technicalguide for obtaining optimal flow velocity recordings. J Am Soc Echocardiogr 10:271–292
Kaul S, Tei C, Hopkins JM, Shah PM (1984) Assessment of right ventricular function using two dimensional echocardiography. Am Heart J 128:301–307
Smith JL, Bolson EL, Wong SP, Hubka M, Sheehan FH (2003) Three-dimensional assessment of two-dimensional technique for evaluation of right ventricular function by tricuspid annulus motion. Int J Cardiovasc Imaging 19:189–197
Tei C, Dujardin KS, Hodge DO, et al (1996) Doppler echocardiographic index for assessment of global right ventricular function. J Am Soc Echocardiogr 9:838–847
Tei C (1995) New non-invasive index for combined systolic and diastolic ventricular function. J Cardiol 26:135–136
Rechtschaffen A, Kales A (1968) A manual of standardized terminology, techniques, and scoring system for sleep stages in human subjects, Brain Information Service, VCLA, Los Angeles, CA
EEG arousals (1992) Scoring rules and examples: preliminary report from the sleep disorders atlas task force of the American Sleep Disorders Association. Sleep 15:173–184
Cicala S, Galderisi M, Caso P, Petrocelli A, D’Errico A, de Divitiis O, Calabro R (2002) Right ventricular diastolic dysfunction in arterial systemic hypertension: analysis by pulsed tissue Doppler. Eur J Echocardiography 3:135–142
Myslinski W, Mosiewicz J, Ryczak E, Barud W, Bilan A, Palusinski R, Hanzlik J (1998) Right ventricular function in systemic hypertension. J Hum Hypertens 12:149–155
Santamore WP, Dell’Italia LJ (1998) Ventricular interdependence: significant left ventricular contributions to right ventricular systolic function. Prog Cardiovasc Dis 40:289–308
Eidem BW, O’Leary PW, Tei C, Seward JB (2000) Usefulness of the myocardial performance index for assessing right ventricular function in congenital heart disease. Am J Cardiol 15(86):654–658
Tuller D, Steiner M, Wahl A, Kabok M, Seiler C (2005) Systolic right ventricular function assessment by pulsed wave tissue Doppler imaging of the tricuspid annulus. Swiss Med Wkly 6:461–468
Mendes LA, Dec GW, Picard MH, Palacios IF, Newell J, Davidoff R (1994) Right ventricular dysfunction: an independent predictor of adverse outcome in patients with myocarditis. Am Heart J 128:301–307
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tavil, Y., Kanbay, A., Şen, N. et al. Comparison of right ventricular functions by tissue Doppler imaging in patients with obstructive sleep apnea syndrome with or without hypertension. Int J Cardiovasc Imaging 23, 469–477 (2007). https://doi.org/10.1007/s10554-006-9168-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-006-9168-6