Abstract
Objective
This study aimed to investigate the correlation of midregional pro-atrial natriuretic peptide (MR-proANP) with severity of septic status in patients with ventilator-associated pneumonia (VAP) and the usefulness of MR-proANP for mortality prediction in VAP.
Design
Prospective observational cohort study.
Setting
University Hospital.
Patients
Seventy-one patients consecutively admitted to ICU who developed VAP. Patients were followed for 28 days after diagnosis, when they were considered survivors. There were no interventions.
Results
MR-proANP levels increased from sepsis to severe sepsis and septic shock on D0 and D4 of VAP (0.002 and 0.02 respectively). Median MR-proANP levels on day 0 and day 4 (pmol/L [interquartile range]) were 149.0 (79.8–480.0) and 249.0 (93.6–571.0) in septic patients, 438.5 (229.3–762.0) and 407.5 (197.8–738.0) in severe sepsis, 519.5 (369.5–1282.3) and 632.0 (476.0–1047.5) in septic shock. On day 0 and day 4, MR-proANP levels were significantly higher in non-survivors (525.0 [324.0–957.8] and 679.5 [435.0–879.5], respectively) than in survivors (235.0 [102.0–535.0] and 254.0 [110.0–571.0], respectively; P = 0.004). Univariate logistic regression model for mortality included age, gender, APACHE II score, creatinine, logarithmic transformed MR-proANP (LnMR-proANP). Mortality was directly related to LnMR-proANP on D0 and D4, with odds ratios (OR) of 2.06 (95% CI 1.21–3.51) and 2.63 (1.33–5.23), respectively. In multivariate logistic regression, only LnMR-proANP D0 with OR = 2.35 (1.05–5.26) and LnMR-proANP D4 with OR = 3.76 (1.39–10.18) remained significant.
Conclusions
Our data demonstrated that MR-proANP levels increase progressively with the severity of sepsis and are independent predictors of mortality in VAP.
Similar content being viewed by others
Introduction
Ventilator-associated pneumonia (VAP) is the leading cause of death from hospital-acquired infections. The estimated prevalence of nosocomial pneumonia in intensive care units ranges from 10 to 65%, with case fatality rates of 13 to 55% [1]. VAP complicates the course of 8–28% of patients receiving mechanical ventilation [2].
Worsening of respiratory failure, the presence of an ultimately or rapidly fatal underlying condition, the presence of shock, inappropriate antibiotic therapy are the factors that negatively affect the prognosis of VAP [3].
In addition to the clinical evaluation, a novel approach to estimate the presence of an infection and to grade its severity and treatment response is the use of biomarkers.
Atrial natriuretic peptide (ANP), a member of the family of natriuretic peptides, regulates a variety of physiological parameters including diuresis and natriuresis, and reduces systemic blood pressure [4, 5]. It is predominantly produced in the atrium of the heart and comprises 98% of natriuretic peptides in the circulation [5]. Mature ANP is cleaved from carboxylterminal amino acids of the prohormone of ANP. The N-terminal portion of the prohormone is secreted in the same molar ratio as ANP [5–7]. Because of its longer half-life, the N-terminal portion of proANP, particularly the mid region of this molecule (MR-proANP) has been shown to be a more reliable analyte [6, 8].
Plasma MR-proANP concentrations have recently emerged as a valuable tool for individual risk assessment in sepsis patients [7]. ANP levels may reflect the inflammatory cytokine response correlated with the severity of pneumonia, as well as the presence of disease-relevant comorbidities, namely heart failure and renal dysfunction [9–13]. ANP levels seem to be more determined by the intrinsic myocardial depression of sepsis. In addition to sepsis-induced myocardial depression, acute lung injury and an increased afterload placed on the right heart following pulmonary hypertension may contribute to cardiac dilation and a rise in circulating ANP [14].
Previous study observed a significant correlation of circulating pro-ANP levels with serum osmolarity and creatinine in septic patients. Non-septic patients with kidney failure revealed mostly normal pro-ANP values, and it is therefore possible that the observed elevation in pro-ANP and creatinine in this study was a result of kidney failure related to sepsis (7).
To date, no published information exists about the behavior of ANP in patients with ventilator-associated pneumonia (VAP).
Our study aimed to investigate the correlation of MR-proANP with severity of septic status in patients with VAP and to analyze the usefulness of MR-proANP as a predictor of mortality in VAP.
Materials and methods
The study was conducted in the clinical/surgical 26-bed intensive care unit (ICU) of the Hospital de Clínicas de Porto Alegre (HCPA), a tertiary-care–teaching institution with 744 hospital beds.
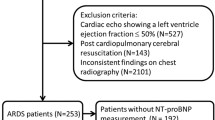
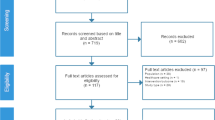
All patients, consecutively admitted to the ICU suspected of VAP were eligible for this prospective observational cohort study. Patients at least 18 years old of age were recruited. Exclusion criteria were a previous diagnosis of AIDS or neutropenia below 1,000 cells/mL. Pneumonia was considered ventilator associated when it occurred after 48 h of mechanical ventilation and was judged to not have been incubating before starting of mechanical ventilation. VAP was considered early-onset when it occurred during the first 4 days of mechanical ventilation and late-onset when it developed 5 or more days later after the initiation of mechanical ventilation [15]. APACHE II [16] was calculated during the first 24 h of admission to ICU. Patients were considered immunosuppressed when they had received chemotherapy within the preceding 45 days, or had neutropenia of less than 1,000/mm3.
Diagnosis of pneumonia was suspected, when a patient developed a new and persistent radiographic infiltrate plus two of the following signs/symptoms: (a) body temperature greater than 38°C or less than 36°C; (b) white blood cells more than 11,000 or less than 4,000/mm3; (c) macroscopically purulent tracheal aspirate [17]. Purulent endotracheal aspirate was defined on inspection by the assistant team. The axillary temperature used was the highest in the previous 24 h, before inclusion into the study.
Chest X-ray, arterial blood gases, complete blood count, creatinine, total bilirubin, and albumin were obtained by the time VAP was suspected (D0) and were repeated on the fourth day of treatment (D4). Quantitative endotracheal aspirate (QEA) was obtained on D0, repeated on the third day after the diagnosis (D3) and then weekly. Sterile endotracheal aspirates were obtained with a suction catheter adapted to a mucus collector without saline instillation, and two samples of hemocultures were collected from different veins with a 15-min interval before starting antimicrobial treatment.
Clinical pulmonary infection score (CPIS) [18], modified as described by Singh and colleagues [19], was calculated on the basis of data on D0 and D3. Patients were assumed to have VAP when the CPIS was 7 points or more. CPIS was calculated with data from D0, adding points for microbiological results and progression of pulmonary infiltrate on a new chest X-ray on D3. To calculate CPIS on D3, data from D3 were used.
For a diagnosis of VAP, there should be no evidence of other medical conditions to which the presenting symptoms, signs or radiological findings could be attributed. A SOFA score was calculated on D0 and D4. QEA was considered positive when values were at least 105 colony-forming units/mL.
All patients with a clinical suspicion of VAP, later confirmed by a CPIS of at least 7 and fulfilling inclusion criteria, were included and they received empirical antimicrobial therapy on D0. The choice of antibiotics and changes rested solely with the critical care team or primary service caring for the patient. Modifications to empirical therapy were based on the results of QEA and hemocultures. Mechanical ventilation, physiotherapy and airway management were performed in accordance with a standard protocol in all patients.
Patients at the time of VAP diagnosis were classified as those with sepsis, severe sepsis and septic shock, which were defined according to international criteria [20, 21].
Patients’ progress was followed until the 28th day (D28) after the diagnosis of VAP. Patients who survived until follow-up were counted as survivors. Patients who died before D28 were non-survivors. Patients discharged from the ICU before D28 were also considered survivors. All patients with VAP were reviewed by one of the investigators to confirm the diagnosis on the basis of predetermined criteria.
Seventy-one patients enrolled from October 2003 to August 2005 constituted the study population. The research protocol was reviewed and approved by the Human Research Committee from the HCPA, and informed written consent was obtained from patients’ representatives before enrollment. The study protocol conforms to the ethical guidelines of the Declaration of Helsinki.
Trained investigators collected data on D0, D3, D4, and weekly until D28. Recorded data included age, sex, cause of ICU admission, arterial partial pressure of oxygen/fraction of inspired oxygen (PaO2/FiO2), APACHE II score, SOFA score, CPIS, co-morbidities including chronic obstructive pulmonary disease, whether active smoker, history of congestive heart failure, history of malignancy, immunosuppression, albumin, use of histamine type-2 receptor (H2) antagonist, use of proton pump inhibitor, use of corticosteroids, dialysis, central vein catheterization, urinary tract catheterization, duration of mechanical ventilation, duration of stay in ICU before VAP, cardiopulmonary resuscitation, intubation (orotracheal versus nasotracheal), and tracheotomy.
Adequacy of the empirical antimicrobial treatment was recorded on the basis of microbiological results. Adequate antibiotic therapy was defined as coverage of all the pathogens isolated (from QEA culture or from blood), by at least one antimicrobial administered at the onset of VAP, determined by the sensitivity pattern in the antibiogram [22]. Treatment was considered adequate when cultures were negative.
Blood was drawn when a diagnosis of VAP was clinically suspected, before empirical antibiotic treatment was started. Samples of serum were prepared and frozen immediately after blood was drawn, then stored at −80°C in the HCPA research laboratory. Assays were performed in batches at the end of the study period.
MR-proANP measurements were performed using an immunoluminometric sandwich assay (B.R.A.H.M.S MR-proANP LIA; B.R.A.H.M.S AG, Hennigsdorf, Germany) as described in detail elsewhere [6]. As a modification to the published assay, the calibration was changed from a synthetic peptide to native pro-ANP in human serum. This modification to the initial description increased precision and dynamics (i.e., signal to noise ratio) of the assay. Details on this modification have been published elsewhere [7].The functional assay sensitivity (defined as lowest value with an interassay CV <20%) is 11 pmol/L. Median MR-proANP in 325 healthy individuals in earlier investigations was 45 pmol/L [6].
Laboratory measurements were performed in a blinded fashion without knowledge of the clinical status of the patient.
Statistical analysis
Continuous baseline data are expressed as mean ± SD. Categorical variables were compared with the Chi square test. Comparison of MR-proANP levels between survivors and non-survivors was analyzed by Mann–Whitney test. Comparison of MR-proANP levels in different septic status was analyzed by Kruskal–Wallis Test. For these analyses, two-tailed tests and P ≤ 0.05 were considered statistically significant. Logistic regression analysis was used to determine the relation of risk factors to clinical outcome. We performed logarithmic transformation of MR-proANP values in the regression models, since they have a non-parametric distribution. In multivariate model, we considered significant variables with biological importance. Variables with P < 0.20 in univariate logistic regression were entered into the multivariate model. In the multivariate model, we considered as significant those variables with P < 0.05. SPSS 11.0 for Windows (SPSS Inc., Chicago, IL, USA) was used for statistical analysis.
Results
Seventy-one patients were included in the study. Forty-five were survivors and 26 non-survivors.
Detailed baseline characteristics of the study population, stratified as survivors or non-survivors, are given in Table 1.
Microbiological identification of VAP is shown in Table 2.
Eight patients were not included in D4 analysis because six patients died before D4, one patient left the ICU before D4 and for one patient MR-proANP measurement was not performed because a serum sample was not available.
Thirty-five of 45 (77.8%) survivors received adequate antimicrobial therapy, compared to 18 out 26 (69.2%) non-survivors (P = 0.57).
Accuracy of MR-proANP to predict mortality in VAP patients on D0 and D4 was assessed by ROC curve analysis. Data are presented in Fig. 1. MR-proANP had a slightly higher accuracy on D4 compared to D0. The AUC for MR-proANP on D0 was 0.71 (SD 0.06; P = 0.004). For a threshold of 489.0 pmol/L (minimal false negative and false positive results), sensitivity was 0.65 and specificity was 0.76. The AUC for MR-proANP on D4 was 0.73 (SD 0.06; P = 0.004). Using a cut-off level of 465.5 pmol/L, sensitivity was 0.75 and specificity was 0.72.
Receiver operating characteristic (ROC) analysis of proANP with respect to mortality prediction in patients with VAP. Data on the day of diagnosis of VAP (D0 left panel) and on day 4 (D4 right panel) are shown. MR-proANP had a slightly higher accuracy on D4 compared to D0. The AUC for MR-proANP on D0 was 0.71 (SD 0.06; P = 0.004). For a threshold of 489.0 pmol/L, sensitivity was 0.65 and specificity was 0.76. The AUC for MR-proANP on D4 was 0.73 (SD 0.06; P = 0.004). Using the cut-off level of 465.5 pmol/L, sensitivity was 0.75 and specificity was 0.72
MR-proANP levels were lower in survivors compared to non-survivors on D0 (P = 0.004) and D4 (P = 0.004). Data are shown in Table 3.
MR-proANP levels at different clinical conditions are shown in Table 4. Patients with late-onset VAP had higher levels than those with early-onset (P = 0.03). The presence of congestive heart failure resulted in higher MR-proANP levels (P = 0.001), but there was no difference in survival between the groups (P = 0.36).
We found correlation between creatinine and septic status (P = 0.04), creatinine and MR-proANP levels (P = 0.0001), and between creatinine and mortality (P = 0.03).
The influence of septic status on MR-proANP levels is shown in Table 5. MR-proANP levels increased from sepsis to severe sepsis and septic shock on D0 and D4 (P = 0.002 on D0 and 0.02 on D4).
Logistic regression analysis was used to determine the relation of risk factors to mortality.
Variables included in univariate logistic regression analysis for mortality were age, gender, APACHE II, Creatinine, LnMR-proANP D0 and LnMR-proANP D4. In univariate analysis, LnMR-proANP on D0 [(odds ratio [OR] = 2.06) P = 0.03] and LnMR-proANP on D4 [(OR = 2.63) P = 0.006] were predictors of mortality. There was a trend to significance for age, gender, APACHE II and creatinine.
Multivariate logistic regression model for mortality included the variables from the univariate analysis. The only variables that remained as independent predictors of death were LnMR-proANP D0 with an OR = 2.35 [(95% confidence interval 1.05–5.26), P = 0.04], and LnMR-proANP D4 with an OR = 3.76 [(95% confidence interval 1.39–10.18), P = 0.01], (Table 6).
Discussion
The current study demonstrated that MR-proANP levels are significantly higher in VAP patients dying within 28 days when compared to survivors. In multivariate logistic regression models of predictors of death including age, sex, APACHE II, creatinine and LnMR-proANP on the day of diagnosis of VAP (D0) and on day 4 (D4), LnMR-proANP turned out to be the only parameter that remained as an independent predictor.
Several studies investigated biomarkers to identify patients at high risk for death in respiratory tract infections. Early identification of patients at high risk may provide an opportunity to change the treatment strategy to improve the outcome.
Procalcitonin and C-reactive protein kinetics were assessed as prognostic markers during VAP, with different outcomes. Increasing procalcitonin values were associated with negative outcomes [23] and decreasing values of procalcitonin and C-reactive protein were associated with survival [24].
Recent studies assessed MR-proANP levels as prognostic biomarker in patients with community acquired pneumonia.
Muller et al. [25] analyzed MR-proANP levels in patients with lower respiratory tract infections to evaluate its prognostic use for the severity of disease and outcome. MR-proANP levels were significantly higher in patients with lower respiratory tract infections when compared with controls, with highest levels in patients with community-acquired pneumonia (CAP). MR-proANP, but not C-reactive protein (CRP) levels, gradually increased with increasing severity of CAP. For survival prediction in patients with CAP, MR-proANP was similar when compared with the PSI, and better when compared with other biomarkers, that is, procalcitonin, CRP and leucocyte count.
Masia and colleagues [26] conducted a prospective observational study of patients with CAP to assess severity of disease. Biomarkers, carboxy-terminal provasopressin (CT-proAVP; copeptin) and midregional proatrial natriuretic peptide (MR-proANP) were measured in 173 patients. They found a positive correlation between pneumonia severity index (PSI) and MR-proANP and between PSI and CT-proAVP. Non-survivors had significantly higher MR-proANP and CT-proAVP than survivors. In multivariate analyses to identify potential predictors of mortality including PSI, procalcitonin, C-reactive protein, lipopolysaccharidebinding protein, CT-proAVP, and MR-proANP concentrations in serum samples obtained at diagnosis, only CT-proAVP remained an independent predictor of death.
Prat and colleagues [27] evaluated the use of midregional pro-atrial natriuretic peptide (MR-proANP) measurement in the stratification of severity in community-acquired pneumonia. Three hundred patients admitted to Emergency Department with CAP were included. Patients were stratified by the pneumonia severity index (PSI), CURB-65 score and by the development of complications. Serum samples were obtained at the moment of admission and prior to antibiotic therapy. MR-proANP increased with the severity of pneumonia, according to PSI score and CURB-65 score. Median MR-proANP levels were significantly higher in patients with high PSI risk class (IVeV) than in those with low PSI risk class (IeIII). MR-proANP levels were also significantly higher in those patients who developed complications or died. There was no association between MR-proANP and etiology of pneumonia and the radiographic extent.
Kruger and colleagues[28] enrolled 589 patients with proven CAP and MR-proANP, CT-proAVP, C-reactive protein (CRP), procalcitonin (PCT) and CURB-65 score were determined on admission. MR-proANP and CT-proAVP were the strongest predictors of mortality. They are significantly lower in CAP survivors and correlate with the severity of the disease measured by CURB-65 score.
Haviv and colleagues [4] performed a study to determine ANP plasma levels in 28 children with pneumonia, compared to levels in 25 children without pneumonia. ANP levels in the pneumonia group (mean ± SD, 16.02 ± 11.69 pg/mL) increased significantly (P < 0.01) when compared to the levels in the control group (mean ± SD, 7.44 ± 9.29 pg/mL), but there was no correlation between ANP plasma levels and severity of pneumonia in their sample.
In contrast, our results showed a significant influence of septic status on MR-proANP levels. MR-proANP levels increased from sepsis to severe sepsis and septic shock both on the day of diagnosis of pneumonia and on the fourth day of treatment. (P = 0.002 and P = 0.02, respectively). We found higher levels of MR-proANP than Haviv et al. We may suppose that our cohort of adults were more severely dysfunctional.
Even though our study involved a different group, ventilated patients with pneumonia acquired in ICU (VAP), our results show great similarity to data presented in the previous studies in CAP patients [25–28]. Our non-survivors group had significantly higher levels of MR-proANP and they gradually increased with increasing severity of VAP.
Morgenthaler et al. [7] studied a cohort of medical intensive care unit patients to compare the prognostic value of MR-proANP levels with those of other biomarkers and physiological scores in 101 consecutive critically ill patients. The prognostic value of pro-ANP levels was compared with that of the APACHE) II score and with those of C-reactive protein, IL-6 and procalcitonin. The median MR-proANP value in the survivors was significantly lower than that in the non-survivors. On the day of admission, MR-proANP levels, but not levels of other biomarkers, were significantly higher in non-surviving than in surviving sepsis patients (P = 0.001).
In the present study, we are unable to compare the prognostic reliability of the MR-proANP with other markers, such as PCT or CRP, and therefore we cannot draw any conclusion regarding which one would be the best prognostic marker.
Our cohort was composed of septic, severely septic or shocked septic patients. It was expected to find high levels of MR-proANP in a group of patients with multiple organ dysfunctions. What we found valuable was the increasing levels of MR-proANP according to the severity of sepsis and the prognostic accuracy for mortality in a group of VAP patients.
References
Guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcare-associated pneumonia (2005) Am J Respir Crit Care Med 171:388–416
Chastre J, Fagon JY (2002) Ventilator-associated pneumonia. Am J Respir Crit Care Med 165:867–903
Torres A, Aznar R, Gatell JM, Jimenez P, Gonzalez J, Ferrer A, Celis R, Rodriguez-Roisin R (1990) Incidence, risk, and prognosis factors of nosocomial pneumonia in mechanically ventilated patients. Am Rev Respir Dis 142:523–528
Haviv M, Haver E, Lichtstein D, Hurvitz H, Klar A (2005) Atrial natriuretic peptide in children with pneumonia. Pediatr Pulmonol 40:306–309
Vesely DL (2002) Atrial natriuretic peptide prohormone gene expression: hormones and diseases that upregulate its expression. IUBMB Life 53:153–159
Morgenthaler NG, Struck J, Thomas B, Bergmann A (2004) Immunoluminometric assay for the midregion of pro-atrial natriuretic peptide in human plasma. Clin Chem 50:234–236
Morgenthaler NG, Struck J, Christ-Crain M, Bergmann A, Muller B (2005) Pro-atrial natriuretic peptide is a prognostic marker in sepsis, similar to the APACHE II score: an observational study. Crit Care 9:R37–R45
Ala-Kopsala M, Magga J, Peuhkurinen K, Leipala J, Ruskoaho H, Leppaluoto J, Vuolteenaho O (2004) Molecular heterogeneity has a major impact on the measurement of circulating N-terminal fragments of A- and B-type natriuretic peptides. Clin Chem 50:1576–1588
Aiura K, Ueda M, Endo M, Kitajima M (1995) Circulating concentrations and physiologic role of atrial natriuretic peptide during endotoxic shock in the rat. Crit Care Med 23:1898–1906
Cowie MR, Struthers AD, Wood DA, Coats AJ, Thompson SG, Poole-Wilson PA, Sutton GC (1997) Value of natriuretic peptides in assessment of patients with possible new heart failure in primary care. Lancet 350:1349–1353
Lubbesmeyer HJ, Woodson L, Traber LD, Flynn JT, Herndon DN, Traber DL (1988) Immunoreactive atrial natriuretic factor is increased in ovine model of endotoxemia. Am J Physiol 254:R567–R571
McDonagh TA, Robb SD, Murdoch DR, Morton JJ, Ford I, Morrison CE, Tunstall-Pedoe H, McMurray JJ, Dargie HJ (1998) Biochemical detection of left-ventricular systolic dysfunction. Lancet 351:9–13
Ruskoaho H (2003) Cardiac hormones as diagnostic tools in heart failure. Endocr Rev 24:341–356
Hartemink KJ, Groeneveld AB, de Groot MC, Strack van Schijndel RJ, van Kamp G, Thijs LG (2001) Alpha-atrial natriuretic peptide, cyclic guanosine monophosphate, and endothelin in plasma as markers of myocardial depression in human septic shock. Crit Care Med 29:80–87
Langer M, Cigada M, Mandelli M, Mosconi P, Tognoni G (1987) Early onset pneumonia: a multicenter study in intensive care units. Intensive Care Med 13:342–346
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: a severity of disease classification system. Crit Care Med 13:818–829
Fabregas N, Ewig S, Torres A, El Ebiary M, Ramirez J, de la Bellacasa JP, Bauer T, Cabello H (1999) Clinical diagnosis of ventilator associated pneumonia revisited: comparative validation using immediate post-mortem lung biopsies. Thorax 54:867–873
Pugin J, Auckenthaler R, Mili N, Janssens JP, Lew PD, Suter PM (1991) Diagnosis of ventilator-associated pneumonia by bacteriologic analysis of bronchoscopic and nonbronchoscopic “blind” bronchoalveolar lavage fluid. Am Rev Respir Dis 143:1121–1129
Singh N, Rogers P, Atwood CW, Wagener MM, Yu VL (2000) Short-course empiric antibiotic therapy for patients with pulmonary infiltrates in the intensive care unit. A proposed solution for indiscriminate antibiotic prescription. Am J Respir Crit Care Med 162:505–511
American College of Chest Physicians/Society of Critical Care Medicine Consensus Conference: definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis (1992) Crit Care Med 20:864–874
Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, Knaus WA, Schein RM, Sibbald WJ (1992) Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 101:1644–1655
Luna CM, Blanzaco D, Niederman MS, Matarucco W, Baredes NC, Desmery P, Palizas F, Menga G, Rios F, Apezteguia C (2003) Resolution of ventilator-associated pneumonia: prospective evaluation of the clinical pulmonary infection score as an early clinical predictor of outcome. Crit Care Med 31:676–682
Luyt CE, Guerin V, Combes A, Trouillet JL, Ayed SB, Bernard M, Gibert C, Chastre J (2005) Procalcitonin kinetics as a prognostic marker of ventilator-associated pneumonia. Am J Respir Crit Care Med 171:48–53
Seligman R, Meisner M, Lisboa TC, Hertz FT, Filippin TB, Fachel JM, Teixeira PJ (2006) Decreases in procalcitonin and C-reactive protein are strong predictors of survival in ventilator-associated pneumonia. Crit Care 10:R125
Muller B, Suess E, Schuetz P, Muller C, Bingisser R, Bergmann A, Stolz D, Tamm M, Morgenthaler NG, Christ-Crain M (2006) Circulating levels of pro-atrial natriuretic peptide in lower respiratory tract infections. J Intern Med 260:568–576
Masia M, Papassotiriou J, Morgenthaler NG, Hernandez I, Shum C, Gutierrez F (2007) Midregional proa-type natriuretic peptide and carboxy-terminal provasopressin may predict prognosis in community-acquired Pneumonia. Clin Chem 53:2193–2201
Prat C, Lacoma A, Dominguez J, Papassotiriou J, Morgenthaler NG, Andreo F, Tudela P, Ruiz-Manzano J, Ausina V (2007) Midregional pro-atrial natriuretic peptide as a prognostic marker in pneumonia. J Infect 55:400–407
Kruger S, Papassotiriou J, Marre R, Richter K, Schumann C, von Baum H, Morgenthaler NG, Suttorp N, Welte T (2007) Pro-atrial natriuretic peptide and pro-vasopressin to predict severity and prognosis in community-acquired pneumonia : results from the German competence network CAPNETZ. Intensive Care Med 33:2069–2078
Acknowledgments
This study was supported by grants from Fundo de Incentivo a Pesquisa, FIPEHCPA, Porto Alegre, Brazil, and was performed in Hospital de Clínicas de Porto Alegre.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Seligman, R., Papassotiriou, J., Morgenthaler, N.G. et al. Prognostic value of midregional pro-atrial natriuretic peptide in ventilator-associated pneumonia. Intensive Care Med 34, 2084–2091 (2008). https://doi.org/10.1007/s00134-008-1173-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-008-1173-x